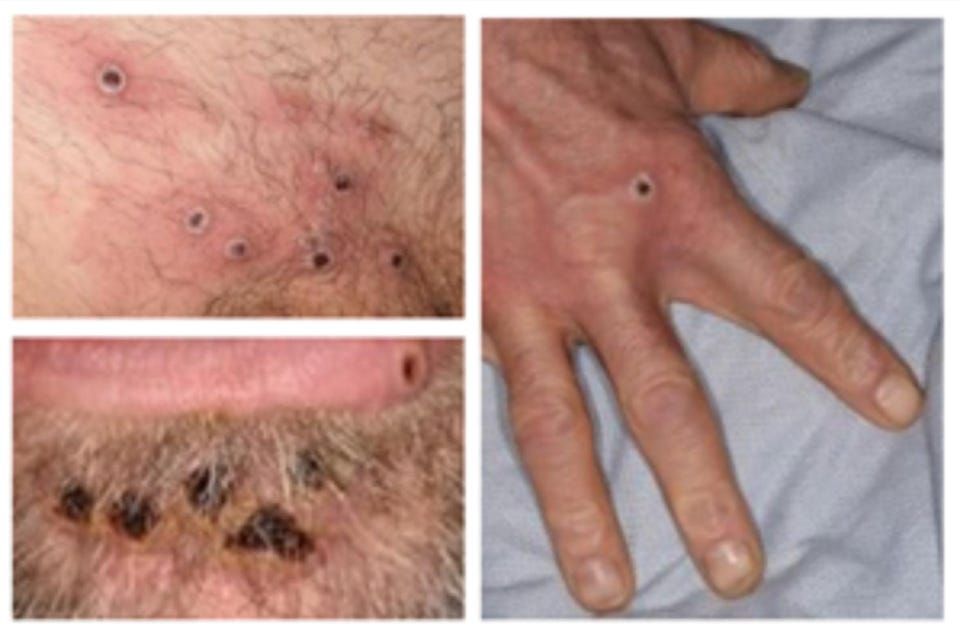
The monkeypox outbreak qualifies as a global health emergency, the World Health Organization’s Director-General Tedros Adhanom Ghebreyesus declared on Saturday, citing a rapid escalation in cases to more than 16,000 reported from 75 nations and territories in recent weeks.
That means the world faces three simultaneous global health emergencies — polio since 2014; COVID-19 since 2020; and monkeypox — that WHO believes deserve a coordinated response, though the U.N. health agency cannot require countries to do anything. Only COVID-19 has been declared a pandemic.